Index
Yeast lives on your skin and in your body. Your immune system usually keeps yeast at bay; however, antibiotic usage, illnesses, and obesity increase the risk of a fungal infection. It’s essential to learn how to avoid chronic yeast infections.

What is a Yeast Infection?
An overgrowth of the yeast Candida albicans causes a yeast infection. This fungal infection affects different body areas, including the skin, mouth, genitals, throat, and blood.
Candida can reside in the digestive tract, mouth, vagina, and skin. Commonly, candida causes no harm; however, if it begins to overgrow, it can cause discomfort. Chronic yeast infections are overgrowths of candida and typically occur in moist areas. A chronic yeast infection is persistent. Here, we look into the various symptoms of chronic yeast infection.
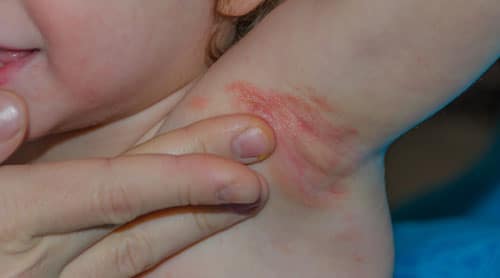
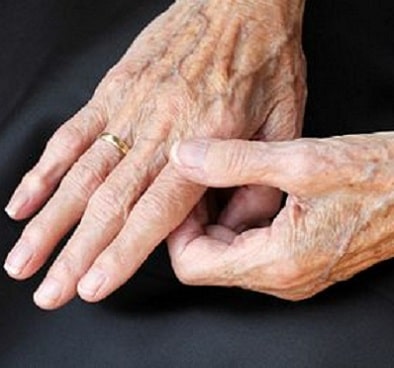
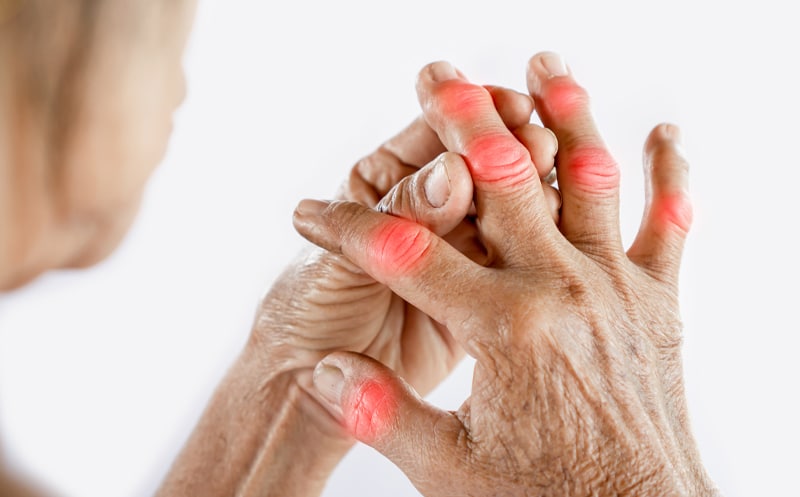
Yeast Infection of Skin
Different fungi and bacteria live on your skin. Most of them do not cause any issues. Many of them are needed to carry out normal skin functions. However, when the fungi and bacteria multiply, a yeast infection of the skin can develop. This condition is also called cutaneous candidiasis or candidiasis of the skin.
The symptoms of a fungal yeast infection of your skin include:
- Irritation and Skin rash
- Intense itching or Redness
- Blister
- Cracked skin
- Inflammation or Painful skin
- Odor
Yeast skin infections can affect any body part and are especially common in the folds of your skin and most areas. The areas that can be affected include under your breast or belly, between your fingers or toes, armpits, abdomen, vagina, uncircumcised penis, or in your groin. You can also develop a yeast infection of the skin around the corners of your mouth or the edges of your nails.
A yeast infection of the skin often presents itself as an irritated rash. The rash will appear red and have scalloped edges. It may be itchy or painful. Many times, parents think their infant has a diaper rash when, in fact, the child has a yeast infection.

Yeast Infection of the Mouth
Oral candidiasis, or thrush, is a yeast infection of your mouth. It occurs when Candida albicans accumulates in the mouth. Candida naturally occurs in the mouth; however, when there is an overgrowth of this fungus, it can cause oral thrush. The symptoms of oral thrush include:
- White lesions on the inner cheeks and tongue
- Thrush can spread to your gums, the roof of your mouth, the back of your throat, and your tonsils
- Cottage cheese-looking appearance on your tongue
- Pain that can make swallowing or eating difficult
- Cracked skin around the mouth
- Loss of taste
- Cottonmouth
- Redness or irritation in the mouth
- At times, white patches (like milk curds) appear on the mouth, lips, or elsewhere in the mouth. Wiping away the white patch may cause bleeding. Thrush is ubiquitous in infants because of the hormone changes experienced right after birth. Research indicates that individuals who have a weakened immune system, cancer, diabetes, medications like steroids (prednisone), and oral conditions can increase the risk of developing thrush. Those suffering from thrush may have pain when eating. Brushing and flossing your teeth twice a day, visiting your dentist twice a year, and limiting the amount of sugary foods you eat can reduce your risk of developing thrush.
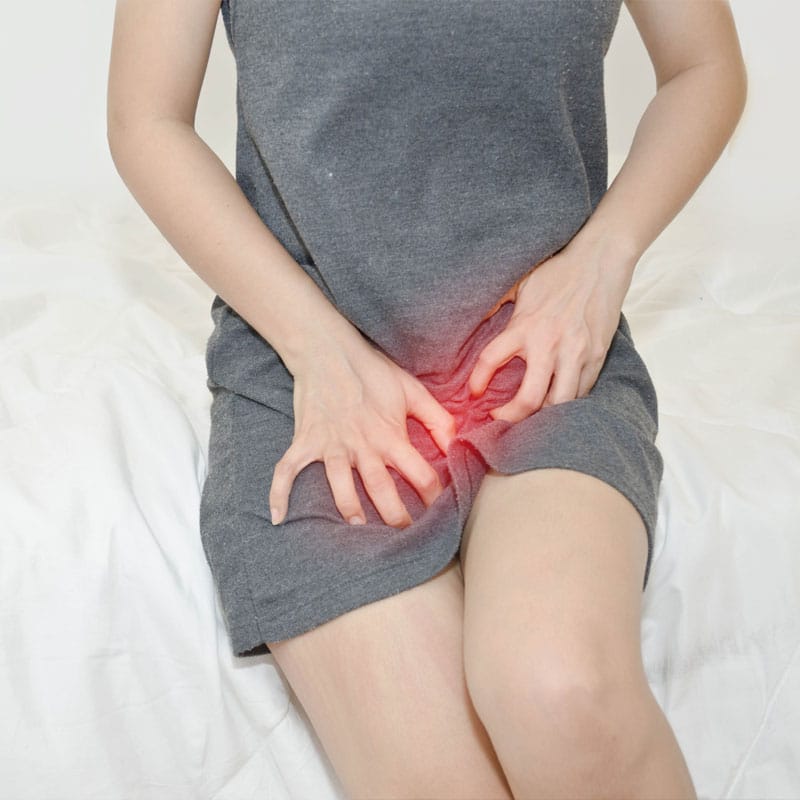
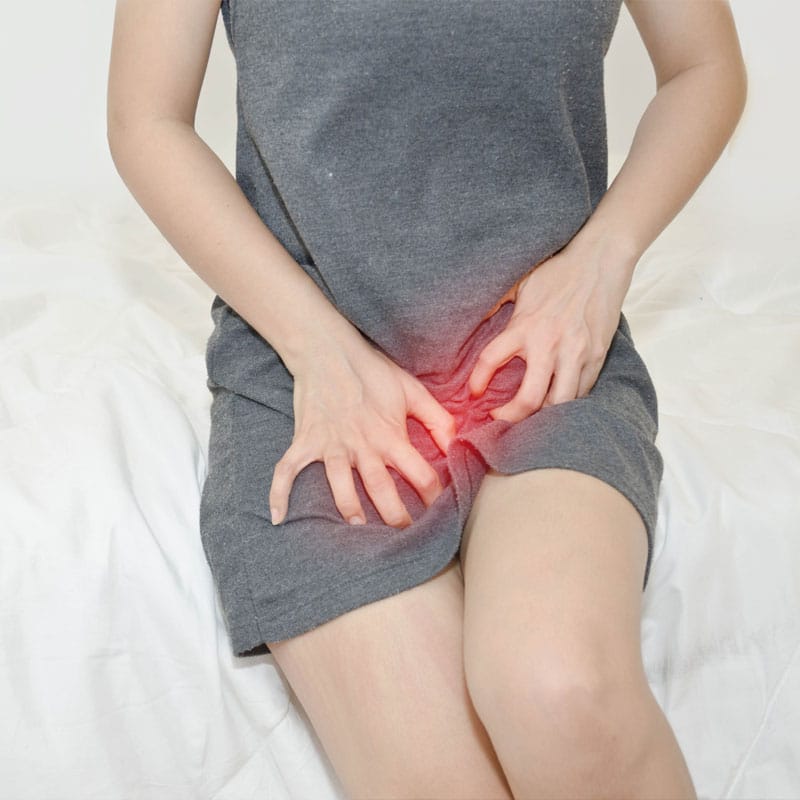
Vaginal Yeast Infection
One of the most common types of yeast infection is a vaginal yeast infection. A vaginal yeast infection results in irritation to the vagina and vaginal area and intense itching. Vaginal discharge may be grayish-white and have the consistency of cottage cheese. Women may experience burning while urinating due to the irritation of the vaginal area.
Approximately 75 percent of women will experience a vaginal yeast infection during their lifetime. Poor hygiene, a compromised immune system, obesity, antibiotic usage, tight-fitting clothing, and pregnancy can increase the risk of a vaginal yeast infection.
Vaginal yeast infections cause a variety of symptoms, including:
- Itching or burning of the vulva and vagina
- Redness/swelling of the vulva
- Vaginal rash
- Vaginal discharge that looks like cottage cheese
- Vaginal pain
- Rash
Invasive Candidiasis
Invasive candidiasis occurs when Candida enters the bloodstream. Patients may experience an atypical fever that does not respond to antibiotic treatment. If the infection spreads to the organs, it can cause serious problems. If left untreated, patients may experience organ failure. Low birth weight infants, patients in intensive care units, and those who have a central venous catheter are at a high risk of developing invasive candidiasis. Finally, HIV/AIDS patients often suffer from chronic yeast infections due to a compromised immune system.

Causes of Yeast Infections
There are numerous causes of chronic yeast infections, including:
- Antibiotics—Antibiotics destroy harmful bacteria and the good lactobacillus bacteria. These bacteria produce acid, making the body inhospitable to an overgrowth of yeast.
- Pregnancy—When women are pregnant, their hormones change, and they have an increased amount of estrogen in their bodies, which can alter the body’s natural pH levels. During this time, Candida can grow out of control.
- Birth control pills—Women on an estrogen hormone therapy routine or a birth control pill that contains high doses of estrogen are more prone to yeast infections.
- Douching
- Diabetes mellitus
- A diet composed of sugars and refined carbs
- Elevated stress levels
- Imbalanced microbiota
- Improperly using catheters
- Increased alcohol consumption
- Weak immune system
Patients using corticosteroids are prone to chronic yeast infections. Finally, yeast infections can be transmitted sexually. If you have any of these risk factors, a change in your diet and some lifestyle modifications can help decrease your risk of a yeast infection.
Holistic Treatment for Chronic Yeast Infection
Patients with four or more yeast infections yearly are often diagnosed with chronic or recurrent infections. Recurrent infections can have many causes, including uncontrolled diabetes, a compromised immune system, and hormonal imbalances.
Our integrative practitioners specialize in treating and preventing chronic yeast infections, skin issues, and other rashes. We focus on treating your whole body rather than just your symptoms. Your diet is essential in reducing the risk of a recurrent yeast infection.